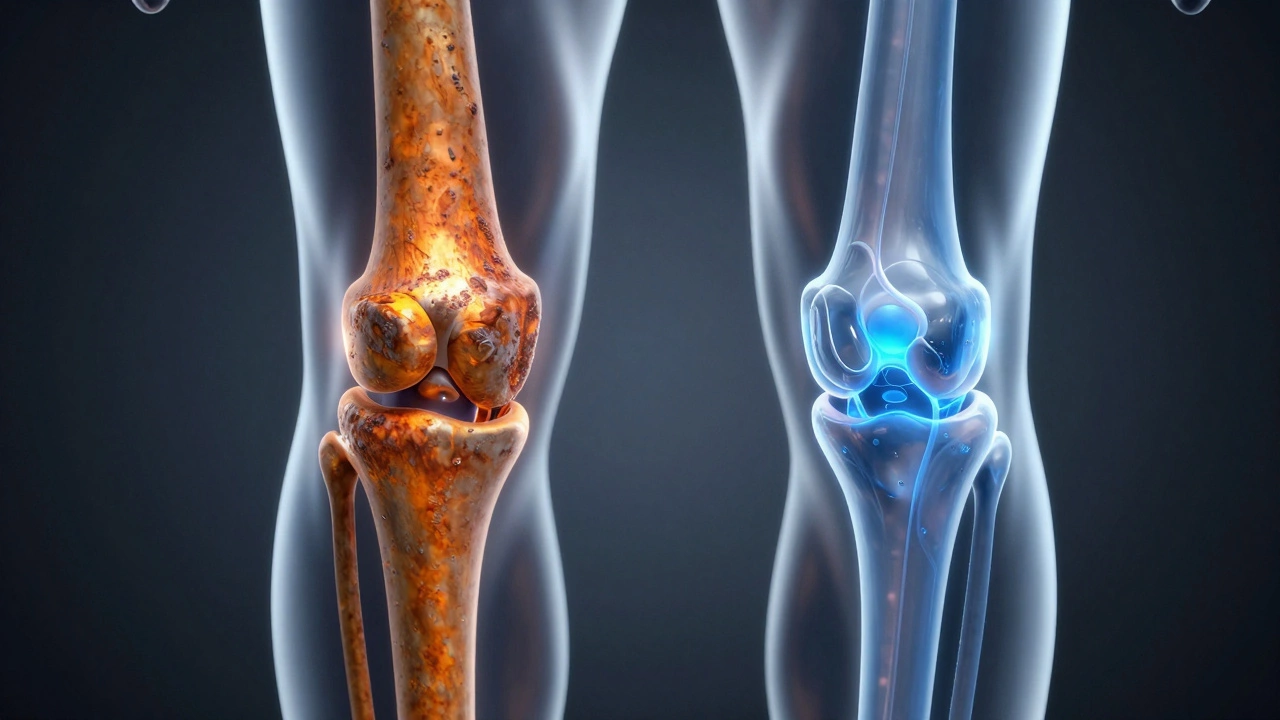
Knee Mobility & Recovery Guide
Identify your stiffness type and get targeted recovery strategies
Your Recovery Outlook
High ReversibilityPrimary Driver: Cartilage Loss
Recommended Strategy:
Select your symptoms and click "Analyze" to see tailored recovery suggestions.
The Real Culprits Behind Stiff Knees
Before you can fix the problem, you have to know why your joint is acting up. Knee stiffness usually falls into a few specific buckets. First, there's Osteoarthritis is a degenerative joint disease where the protective cartilage on the ends of your bones wears down over time. When that cartilage disappears, bone rubs against bone, causing inflammation and a feeling of tightness. Then you have post-surgical stiffness, often seen after a Knee Replacement is a surgical procedure to replace a damaged or worn-out knee joint with an artificial prosthesis. In these cases, the stiffness isn't from cartilage loss, but from scar tissue-also known as adhesions-forming around the joint.
Other triggers include Rheumatoid Arthritis, which is an autoimmune disorder that attacks the joint lining, and ligament injuries like a torn ACL. When the joint is injured or inflamed, the body produces extra synovial fluid. While this fluid is meant to lubricate, too much of it (joint effusion) can actually make the knee feel tight and limit your range of motion. If you feel like your knee is "full" or swollen, you're fighting fluid, not just stiffness.
If your stiffness is caused by inflammation or mild arthritis, you can absolutely reverse the feeling of tightness. The goal here is to break the cycle of "stiffness leads to inactivity, which leads to more stiffness." Movement is the only way to signal to your body that the joint needs to remain mobile. Physical Therapy is the gold standard here. A therapist doesn't just give you exercises; they use manual therapy to glide the joint and stretch the surrounding muscles.
One common mistake people make is avoiding movement because it hurts. While you shouldn't push through sharp, stabbing pain, a dull ache is often a sign that you're breaking through that "morning rust." Low-impact activities like swimming or cycling are game-changers because they move the joint through its range of motion without the pounding force of walking on concrete. Think of it as a gentle massage for the joint from the inside out.
To reverse stiffness, you need to focus on Range of Motion, which is the full movement potential of a joint, usually measured in degrees of flexion and extension. If you can't fully straighten your leg (extension) or bend it enough to touch your calf to your thigh (flexion), you have a ROM deficit. This deficit creates a snowball effect: your muscles atrophy because they aren't being used, and the joint capsule tightens further.
To fight this, focus on "active" and "passive" stretching. Active stretching is when you use your own muscle power to move the joint. Passive stretching is when you use a strap or your other leg to push the joint further. For someone recovering from a knee replacement, achieving full extension-getting the leg completely flat-is often more critical than flexion. If you can't straighten your leg, you'll always walk with a slight bend, which puts massive stress on your hip and lower back.
Sometimes, the stiffness is a result of a mechanical blockage or severe bone-on-bone contact that no amount of stretching will fix. This is where medical interventions come in. Corticosteroids can be injected directly into the joint to kill off inflammation quickly, providing a "window of opportunity" where the pain is low enough for you to perform aggressive physical therapy.
Another option is viscosupplementation, where a hyaluronic acid gel is injected to mimic the joint's natural lubrication. It's like adding high-grade oil to a creaky machine. However, if the joint is completely destroyed, the only way to truly "reverse" the stiffness and regain a functional life is through knee replacement. Once the worn-out biological joint is replaced with a prosthetic, the mechanical cause of the stiffness is gone-though you still have to deal with the surgical scar tissue through rehab.
Once you've regained some mobility, the challenge is keeping it. Stiffness loves stillness. If you spend eight hours a day sitting at a desk, your joints are essentially freezing in place. Use the "20-minute rule": every 20 minutes, stand up and perform five gentle knee bends. This keeps the synovial fluid circulating, which nourishes the cartilage and keeps the joint lubricated.
Hydration also plays a massive role. The tissues in your joints are largely made of water. If you're dehydrated, your joint lubrication becomes thicker and less effective, making that "creaky" feeling more pronounced. Pair this with a diet rich in Omega-3 fatty acids, found in fish oil or walnuts, which naturally helps dampen systemic inflammation.
In your quest to reverse stiffness, don't fall into the trap of "no pain, no gain." There is a big difference between the stretching tension of a tight muscle and the sharp, electric pain of a joint injury. If you feel a pop followed by immediate swelling, stop immediately. Pushing through a meniscus tear or a ligament sprain can lead to permanent joint instability.
Avoid high-impact activities like running on concrete or jumping rope until you have a baseline of strength. If your knee is stiff, your shock absorbers aren't working. Forcing a stiff knee to handle high-impact loads is a shortcut to needing a replacement surgery much sooner than you'd like. Stick to the elliptical or a stationary bike until your ROM is back to a functional level. It depends on the cause. For simple inflammation or inactivity, you might feel a difference in 2 to 4 weeks of consistent movement. However, for post-surgical scar tissue or advanced osteoarthritis, it can take 3 to 6 months of dedicated physical therapy to see significant gains in range of motion. For stiffness, heat is generally better. Warmth increases blood flow and relaxes muscles, making it the perfect pre-stretch tool. Use ice only after a workout or when there is active, visible swelling to bring down inflammation. The evidence is mixed. Some people report a reduction in stiffness, while large-scale clinical trials show limited effectiveness. They aren't a "cure," but they may provide mild support for some users when paired with exercise. This is called "gel phenomenon." During sleep, the synovial fluid in your joint thickens and settles. As you move, this fluid warms up and redistributes, which is why the stiffness usually eases after a short walk or a warm shower. See a professional if your knee "locks" (you physically cannot move it), if the stiffness is accompanied by a fever, or if you experience a sudden loss of stability where the knee gives out during a normal walk.Can You Reverse It Without Surgery?
Cause
Primary Driver
Reversibility Level
Best Approach
Osteoarthritis
Cartilage Loss
Manageable / Partial
Weight loss, PT, low-impact exercise
Post-Surgical Scarring
Adhesions
High (with effort)
Aggressive stretching, Manual therapy
Rheumatoid Arthritis
Autoimmune Attack
Cyclical
Medication (DMARDs) + Movement
Joint Effusion
Excess Fluid
High
Compression, Drainage, Anti-inflammatories

The Role of Range of Motion (ROM)
When Movement Isn't Enough: Medical Interventions

Daily Habits to Keep Stiffness Away
The Danger Zones: What to Avoid
How long does it take to reverse knee stiffness?
Is heat or ice better for stiff knees?
Can supplements like glucosamine actually help?
Why is my knee stiffer in the morning?
When should I see a doctor about my stiffness?